Images of pellucid marginal degeneration
A +2.00 add resulted in visual acuities of 20/20 OD and OS at both distance and near. Cover test confirmed an 18 prism diopter constant alternating exotropia at distance and near.
IMAGES OF PELLUCID MARGINAL DEGENERATION FULL
Extraocular muscles were full with no restrictions. The patient’s pupils were equal, round and reactive to light and accommodation without afferent pupillary defects OD, OS. He did not present with glasses therefore, all visual acuities were taken without correction. The patient’s entering visual acuities were OD 20/50- distance and 20/25- near, and OS 20/20- distance and 20/40 near. The patient was oriented to time, place and person, and his mood and affect were appropriate. Family history included a paternal grandmother who had type 1 diabetes, a sister who had suffered a stroke, and a father who was hypertensive. Blood pressure was taken in-office from the right arm with the patient in a seated position and measured 120/78 mmHg. The patient stated that he had never been a smoker, did not currently drink, and did not use any recreational drugs. His only reported allergy was to penicillin. His current medications and supplements included glucosamine, methylsulfonylmethane (MSM), fish oil and turmeric. His history also included occasional mild joint pain. The eye discoloration was present before the round of antibiotics. The patient’s medical history included a recent tooth abscess for which he underwent a root canal and finished a round of antibiotics. The only significant ocular diagnosis at that examination was an alternating exotropia. His last eye exam was approximately 10 years ago. He did have longstanding floaters with no recent changes or increase in number. He reported no other problems such as eye pain, flashes, photophobia, diplopia, headaches or trauma. She noticed this “discoloration” about one month earlier. He complained that his wife had noticed some coloration changes “on his right iris” in the upper quadrant.

The patient, a 52-year-old Caucasian male, was seen at the clinic for a comprehensive ocular examination.
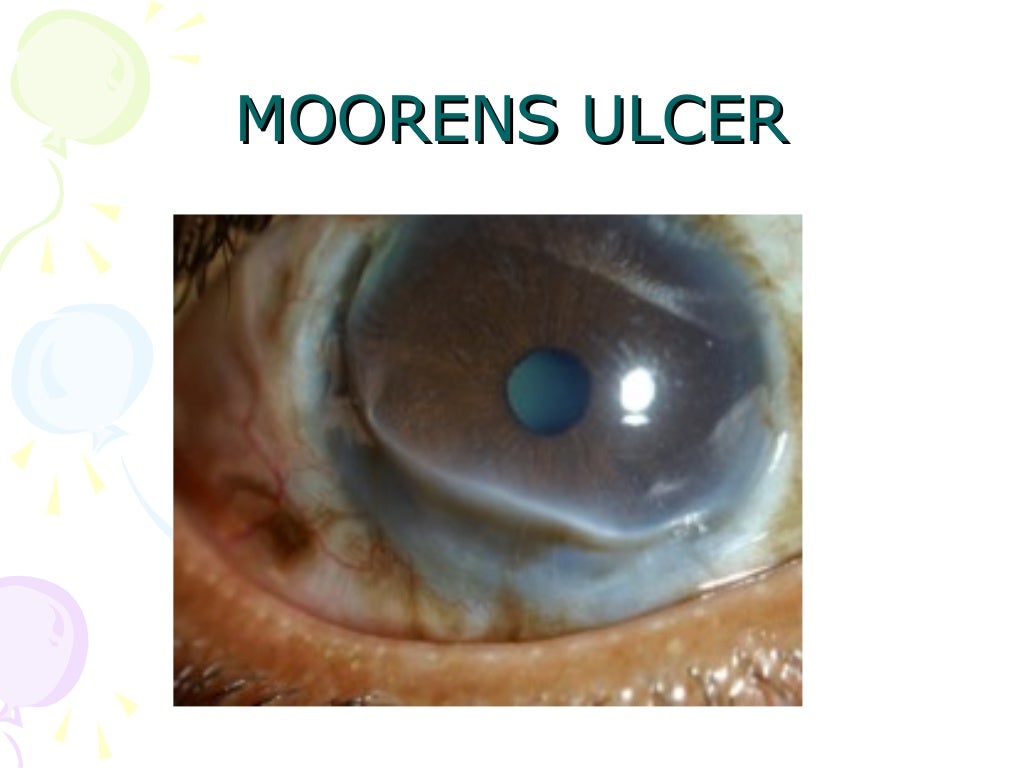
Stromal opacities in the superior cornea OD.

For third- and fourth-year students and residents, the same concepts can be stressed, with the addition of differential diagnosis and treatment and management of patients with TMD.įigure 1. For first- and second-year students, emphasis can be on corneal structure and diagnostic testing that can be performed. This teaching case report is intended for optometry students at all levels. Patients are often asymptomatic but may complain of mild irritation or vision changes due to increasing against-the-rule or oblique astigmatism. Perforation of the cornea is rare but may occur spontaneously or secondary to trauma. The condition is often bilateral and asymmetric. With progression, a gutter forms in the affected area due to stromal thinning, leaving the epithelium intact. Initially, TMD presents as small, yellow-white, stromal opacities composed of lipids with some superficial vascularization, which begins superiorly and spreads circumferentially. The condition is most commonly seen in males past the age of 40. Terrien’s marginal degeneration (TMD) is a rare, slowly progressive, peripheral corneal ectasia of unknown etiology.
